Welcome to the Virtual MS Center!
Ask any question you want about Multiple Sclerosis and one of our experts will answer it as soon as possible.
|
Here is My Question:
Do I really need another MRI? Over past three years I have been followed by specialist and symptoms have been minimal: tingling, heat insensitivity and chronic fatigue for which I take mess. During this time I was also dx'd with optic atrophy from optic neuritis but again symptoms were subacute. I have had 3 Brain mris. First showed 4 nonspecific white matter changes, with second some had disappeared and with third I was told it was possible to count 8, still nonspecific but radiologist still reports as normal MRI. So now I have to have a 4th a year later. Is it worth it? I mean from point of view of expense as well as exposure to contrast- I have also had spine mris which showed nothing. Is there a real chance I could have MS or am I being followed from an excess of caution? Is another MRI the way to go or would you suggest other testing or nothing? I would really welcome your advice as I am feeling very unsure. Answer: I can understand why you are perplexed. For instance, I would never tell a person with MS that they have “8 lesions” and then turn around and say their MRI is normal. It is possible for an MRI to display innumerable non-specific white matter hyperintensities but this would not be supportive of a diagnosis of MS. The ultimate question is why are your physicians obtaining MRI scans on a regular basis. It sounds as if they are not at all certain of the diagnosis. If this is the case, spinal fluid analysis is quite useful. This is done with a procedure called a lumbar puncture or “spinal tap.” If it is felt that your MRI has not shown any significant changes over 3 years (this is a big if), there is little reason to repeat MRIs frequently. My practice is to obtain monitoring MRIs at 6, 18 and 36 months then 5 and 10 years in people with symptoms and findings consistent with MS (such as your residual optic atrophy) but minimal evidence to support an active diagnosis. Clinical re-evaluations are done on a yearly basis and we move up an MRI scan if we believe the disease has become clinically active. I would never treat an individual without stronger evidence to support a diagnosis of MS. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
So I have been somewhat diagnosed with MS (not sure how severe as of yet) there are lesions noticeable however I have had to lumbar punctures and the fluid has come back negative. The Dr. has started me on Copaxone (Glatopa) 20 mg. Just wondering if there is any reason I shouldn't drink alcohol? Chris Answer: There is no problem with drinking alcohol in moderation. As for starting Glatopa, what is the goal of this treatment? This may seem like a silly question, but if your doctor is not even sure of the diagnosis why is it being prescribed? Were you given the option of monitoring your condition with regular MR imaging to determine: a) Do you have MS?; b) How active is your MS?; and c) Does it require treatment? While I do not know the details of your case, these are the questions that all patients must ask before initiating treatment since day to day symptoms are not likely to abate on treatment with Glatopa. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Question:
I switched from Tysabri to Tecfidera 18 months ago. Had a 2-month wash-out from Tysabri, then cortisone one a month for 3 months. Started Tecfidera after the 2-months wash-out. 2 wks 140 then full dose. Starting experiencing severe lymphopenia at month 6. Now at month 16 dropped down to 586. Should I stop Tecfidera considering my average lympho count has been 600 for 13 months. I was offered Aubagio but I'm fearing hepatic problems (had hepatic problems leading to stop Gylenia) and hair loss. How long is the recommended wash-out ? Thank you. Marie Answer: I’ll handle each of your questions separately since they are not related: 1. How long is the recommended wash out on Tysabri? There is no recommended wash out period. I prefer to start patients on an alternative Disease modifying therapy (DMT) as soon as possible to avoid a relapse during the Tysabri withdrawal period which is common in the first 6 months after stopping Tysabri. It often takes time for DMTs to become fully effective and the longer you wait to start a new DMT, the higher the likelihood you will experience a relapse. You would not start another DMT immediately after stopping tysabri, if there is any concern you could have either symptomatic or presymptomatic PML. This is why we always obtain a repeat MRI of the brain before starting a new DMT and then repeat the MRI 3 months later. 2. How do you know when you to stop Tecfidera because of a low lymphocyte count? This is an area of controversy right now. All agree that persistent (a few months) Lymphocyte counts below 500 should prompt you to stop treatment. I personally recommend stopping Tecfidera with lymphocyte counts below 600 lasting for more than 3 months. Since Lymphocyte counts tend to remain low or drop further, especially in people over 55, I tend to halt treatment, at least temporarily, in patients with lymphocyte counts between 600 and 800 with large drops in CD8 counts (a type of lymphocyte subset), if persistent for more than 6 months. The concern is that lymphocyte counts may fail to recovery if they persist too long. Discuss your concerns with your MS specialist and the options available to you. Only your MS specialist knows enough about the details of your illness to assist you with treatment decisions. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego PLEASE NOTE: The information/opinions on this site should be used as an information resource only. This information does not create any patient-HCP relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition. #Tecfidera #Tysabri Here is My Question:
I am concerned of the risk of the onset of progressive multifocal leukoencephalopathy (PML) over the long-term. I was prescribed Tysabri for 8 months, than stopped after a flare-up which lead me to be hospitalized & a round of steroids. I was than switched to Tecfidera & after a year, the standard blood work resulted in "concerns" by my specialist. Additional blood work after the JCV test, I was found positive. So no new generation DMDs will be prescribed by my specialist due to these concerns. My concern is even though I have stopped using such, given the fact I am positive for the JCVirus, is there a risk that has been put into action which could lead to PML down the road? I was told once by my specialist once that these new DMDrugs could put these "side effects" into play either on the 1st dose or the 20th - no one knows for sure, as they are new drugs & not in use long enough to know the long-term impacts. I know I may get back the same answer but maybe others may have researched this further. I know the prognosis is not good if you do get such, but how long must one consider this hurdle & continue to watch for signs. Should I continue to have my blood work monitored? Thanks for any help! Answer: I would really encourage you to read some of information on our website concerning the risk of PML (just type in "PML" in the search box in the upper right corner on this page), because most of the statements and assumptions mentioned in your question are incorrect. Let me briefly summarize for you. 1. A positive JCV antibody test is a risk factor for the development of PML on Tysabri therapy ONLY. It is not a risk factor for PML on other disease modifying therapies, probably because the risk of PML on other disease modifying therapies is so low. 2. No one has developed PML more than 6 months after stopping Tysabri. It is assumed, for good reason, that most people diagnosed with PML after stopping Tysabri probably developed the PML during the Tysabri treatment period. The PML in these cases was only detected several months later when it became symptomatic. 3. The risk of PML on Tysabri therapy does not become significant until a person has been on Tysabri for more than 2 years. This risk is partly dependent on the titer or amount of JCV antibodies measured in your testing. Those with a JCV antibody index > 1.0 have a higher risk of PML after 2 years of therapy. Remember, the risk of PML in the highest risk patient after 2 years of therapy is still only 1 in 100 or 1 percent. This is a pretty low risk, and a risk that many highly active MS patients will take if other options have not been effective. It is increasingly recognized that diligent clinical and MRI monitoring in high risk patients can detect PML early (presymptomatic) with very good outcomes after stopping Tysabri. 4. The risk of PML on Tecfidera and other DMTs is exceedingly low. There are fewer than 10 reported cases of PML on tecfidera or related compounds over the past 20 years. The only known risk factor for PML on Tecfidera is a sustained lowering of the absolute lymphocyte count below 500 to 600. This is why we recommend discontinuing Tecfidera if blood testing over several months reveals a sustained lowering of the absolute lymphocyte count to these low levels. As with Tysabri, it takes a long time for PML to develop while receiving therapy with tecfidera unless your are immunocompromised when you start on treatment. Within several weeks or months of stopping tecfidera, your lymphocyte count should return to normal and your risk of PML should become negligible. Ultimately, the best therapy for you will depend on the stage of your disease and your risk factors for disease progression. If you are considered a person at high risk for significant MS disease progression over the next 5 years, you require highly active therapy. These therapies have some risks but these risks often pale in comparison to the risks associated with progressing disease. Your MS doctor may consider you a low risk for getting significantly worse in the next 5 years. If this is the case your may simply benefit from an injectable therapy or Aubagio . If he considers you high risk, then you should consider an intermediate (Tecfidera or Gilenya) or highly active (Tysabri, Lemtrada, Rituximab) therapy. If you have a difference of opinion on this subject, you may benefit from a second opinion to clarify your situation. Good luck Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
I'm an elderly urban female with a childhood history of pertussis, histoplasmosis, and lots of pneumonia. Neuro symptoms at eighteen began with permanent severe fatigue, mild muscle soreness, and permanent loss of driving reaction time. Two years later--trigeminal neuralgia. Eight years later--two incidents of idiopathic (three week) hearing loss years later--two year disorientation. Permanent stiff neck. Hand tingling. Increasingly marked walking difficulty. Recent difficulty producing speech sounds and (oddly) hearing speeded up speech on electrical devices. (I'm using subtitles.) When I read and speak, the rhythm sounds like metrics now. One online site said it's MS or a brain tumor. I had a clear brain scan two years ago and have scheduled a Tesla 3 scan for Early November. My internist suspects MS (once diagnosed by a vascular specialist)" but with no examination the neurologist said one in a million chances lesions wouldn't have on the previous (two year old) scan. His 'exam' was having me shut my eyes without falling. He strongly suggested CFS, but the only symptom I have on the CFS llists is fatigue. No 'brain fog' problems. No lymph node swelling, etc. Opinion? Answer: It would be most unusual to experience MS for many decades without developing abnormalities on MR imaging. That being said, I am often told that an imaging study is normal or only reveal non-specific white matter hyperintensities, only to find on personal review that the MRI is anything but normal. There is also a strong possibility that this is not MS. The only symptom you experienced that is specific for MS is the Trigeminal Neuralgia. This is also frequently misdiagnosed and turns out to be migraine or trigeminal autonomic cephalgia or atypical facial pain. I would suggest seeing an MS specialist if you are concerned. After so many years, if you have MS it is certainly a relatively mild form of the disease; but I can certainly understand your interest in trying to understand the symptoms you’ve experienced off and on for so many years. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego  Here is my question: I have been reading about the impact of the 'gut' on MS. Are we really what we eat? What is your opinion about this and what can I do NOW in regard to eating that will help my symptoms? Answer: What we eat has a significant impact on our health, regardless of whether we have MS or not. Here is a blog I wrote a while back that should answer your question: READ BLOG Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
I was just diagnosed with RR MS and my doctor is talking about treatment with one of these medications: Tecfidura, Aubagio and Copaxone. In reading about these treatments on your page - my understanding is that they are only to prevent me from getting worse/relapsing, but they won't help me to feel better day to day and with side effects - I may feel worse? Is this correct? Thank you. Answer: It is always important to establish appropriate goals when you start a treatment for your MS. This helps alleviate some of the concerns that you’ve expressed in your question. But let’s discuss some concepts first. Your question seems to imply that if a treatment doesn’t make you feel immediately better, it is not worth taking the treatment. This could not be further from the truth. Many of the persistent symptoms you are experiencing exist because the disease has been active and at least partially damaging your nervous system. This process is likely to continue without treatment. We tend to view symptom management and disease management separately. Symptom management involves a number of approaches (including physical therapy, orthotics, aerobic exercise, progressive resistance training, dietary adjustment, cessation of smoking and other vices, elimination of offending medications, judicious use of some medications to modify symptoms, treatment of co-morbid conditions, meditation, yoga, acupuncture etc) used to modify if not eliminate a particular problem. Disease management is designed to prevent further damage and symptoms from appearing. When you do pick a disease modifying therapy you need to really consider three phases of treatment separately: Phase I: This is the first 1 to 3 months of treatment when you are most likely to experience potential side effects of the treatment. Some treatments like Tecfidera tend to cause side effects early in treatment (4-6 weeks) and then the side effects diminish, if not disappear in most patients. Other therapies like Copaxone may continue to create the same side effect as long as you remain on treatment, notably injection site discomfort and skin reactions. Aubagio can cause hair thinning early in about 1 in 10 people, but this typically resolves within 6 months. Knowing the time course of these side effects and how to manage them is extremely important for making treatment decisions and dealing with whatever side effects emerge. Phase II: This phase generally goes from month 3 to month 18. By this time you should know if you will be able to tolerate the treatment . Now you need to find out if the treatment works. Your neurologist should obtain a new baseline MRI scan of the brain 3 months after starting the treatment (if you plan to continue the treatment). Subsequent MRI scans 9 and 18 months after starting treatment (some neurologists do these scans 12 and 24 months after starting treatment ) can be compared to this baseline scan to see if the treatment is eliminating MRI related disease activity. If the treatment is not eliminating new MRI disease activity, it is probably time to consider a new treatment. Relapses during this time would also be a reason to consider an alternative treatment. Phase III: This phase goes from about 18 month to 36 months. During this time you will be trying to determine if the treatment is continuing to eliminate MRI activity and relapses but, more importantly, you want to know if the treatment is limiting the development of brain atrophy and worsening disability. This usually requires your doctor to use special quantitative clinical and imaging measures. It is also during this phase that the rare long term risks of some of the more powerful therapies (alemtuzumab and Tysabri) emerge. Your doctor must be vigilant and monitor you for these risks at a time when you are feeling quite comfortable with the therapy. I hope this helps with your decision process. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
Are allergy shots safe when you have MS? Also, is potent curcumin safe? It has immunomodulatory effects. Thank you. Answer: I know of no evidence that allergy shots create any harm in MS patients and they are not contraindicated in MS. I must admit, however, that few of my adult MS patients have ever reported taking allergy shots. The active ingredient in Turmeric is curcumin. Please read my previous answer on this subject at the following link http://www.healthcarejourney.com/q--a-for-virtual-ms-center/may-19th-2015 Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
I have been dx with RRMS for 2 year; I have been on Copaxone since diagnosis and Rituxan for another medical condition - Ocular inflammatory syndrome which is significantly improved on Rituxin. However, I've had a mild to moderate relapse on both drugs. I am considering staying on combo- but there is thought to moving on? What is your advice if could generally comment. I am considering Lemtrada. The ophtho would have to agree. Exercise, diet and spirituality are my coping methods. Thank You. Answer: It is hard to answer your question without knowing the details of your case. For the purpose of my answer I will assume you have an average case of MS and received the usual dose of rituximab (1000 mg IV X 2 doses every 6 months) in addition to the copaxone. Given these assumptions here are some issues to consider: Alemtuzumab is a great drug but causes prolonged immunosuppression and a significant risk of autoimmune disease (involving thyroid, platelets and kidneys). All of these issues can be managed. The bigger concern with someone early in the onset of MS , especially if they are relatively young with an uncertain chance of significant worsening over the next 5-10 years, is the potential for long term direct and indirect negative consequences of this treatment ? For instance, how long can you be treated and retreated with alemtuzumab and will this lead to other complications related to prolonged immunosuppression? What if you require other treatments, such as Tysabri, in the future? We know that a prior history of immunosuppression increases the risk of developing progressive multifocal leukoencephalopathy (PML) on Tysabri therapy. Therefore, treating with alemtuzumab first would create greater risks on Tysabri and potentially other DMTs as well. I would only consider Alemtuzumab in your case if I thought it likely that your disease would significantly worsen and limit your activities and ability to work and function within the next 5 years. Otherwise, I would consider an alternative disease modifying therapy. I hope this helps in your decision making. You will need to discuss your risk factors for near term disease progression with your MS specialist before you will be able to make this decision wisely. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego PLEASE NOTE: The information/opinions on this site should be used as an information resource only. This information does not create any patient-HCP relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition. Here is My Question:
I've been injecting Copaxone 20 mg and then it's generic form for three months now (newly diagnosed RR). I have also become incredibly sick with a virus one month (lasted five days), and bacterial infections (upper respiratory, eyes; lasting 5-7 days) the subsequent two months. I've also had a week of relapses all three months. My understanding was Copaxone/Glatopa was not an immune suppressant but was instead supposed to increase the amount of healthy white blood cells and their action in my immune system, reduce relapse rates and slow lesion/disease progression. Instead, I feel as if everything's becoming worse in my body. What is happening? How can I be this sick with a virus or bacterial infection monthly, continue relapsing (though I'm relapsing a bit less) and have any sort of life? Is this common for users of this drug? I'm beside myself. Answer: There are many potential explanations for the recurrent infection but without knowing the details of your case it is hard for me to comment. What I can tell you is the following: 1. Copaxone or Glatopa does not suppress your immune system and I doubt it is responsible for the prolonged infection 2. Steroids can suppress your immune system, so if you received steroids in the past 3 months this may be your explanation 3. All disease modifying therapies like Copaxone take time to start working. It is not unusual for people to relapse in the first few months on treatment. It is the relapses beyond the first three months of treatment that create greater concern that the drug will not be effective if continued Good luck Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
How easy is MS to diagnose? After someone has an attack and they do an MRI of brain and spine, how easy are the lesions to see? If early in disease then how long would they take to show up? After 2nd attack or time frame? Answer: Generally MS is hard to diagnose with confidence early except in cases with very typical syndromes and typical MRI findings. This probably occurs in less than half of the patients in whom the diagnosis is initially considered. As many as 25 % of patients referred to tertiary MS Centers with a diagnosis have another condition or a rare variant of MS. Read through our diagnosis page on this website. Here is the link DIAGNOSIS PAGE as it has lots of information that might further answer your question. Also, in the search box in the upper right corner of the page, there is a search box. Type 'diagnosis' in this box and you will see many posts regarding the topic of diagnosis. Also, in the column to the right on this web page there are topics and you can click on 'diagnosis' to see all the many questions we have received regarding diagnosing MS. Scott Nielsen, MD wrote a blog about how long it takes to get a MS diagnosis that you might want to read as well READ MORE Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
So, I am up to 4 lesions on my brain now. My doctor wants me to start on a DMD. He is hoping to start me on Tysabri, but there is a risk of PML so I am having a blood test for the JC virus in the morning. I was wondering what your thoughts were. He's also considering Copaxone, Aubagio or Avonex and has kind of left it up to me to choose. Any insight would be a blessing. Answer: It is somewhat hard to provide advice given the information you’ve provided but let me give you some information to help you think through the process of making a treatment decision 1. The average person with MS has more than 4 lesions on MRI when they present with their first symptoms of MS. 2. I am assuming you have few outwardly apparent problems from MS which you be typical for someone early in the course of the disease. How MS is affecting you at present is not stated in your question 3. There are no validated treatment effect modifiers for any of the disease modifying therapies. This means that there are currently no tests or features that tell us whether a person will respond to a particular treatment . The only current treatment modifier is a progressive disease course. Progressive disease is a negative modifier meaning that this predicts non response to all current treatments. 4. All the DMTs mentioned in the list are potential treatment options for a person who has never been on treatment. Given the information provided I am not sure I would consider Tysabri even if you were JC virus antibody negative, but your MS specialist probably knows more about your case. That leaves you with Avonex (a once a week injection with flu like side effects), Copaxone (a daily or three times a week injection that hurts and causes skin reactions in many) or Aubagio (a pill that is generally well tolerated but may cause a little hair thinning for a while and requires some monitoring blood tests for a few months). This is a situation where it is nice to have choices. The last three options mentioned are remarkably safe, so start with the one that fits your lifestyle best. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
What are Plegridy's ingredients? Answer: Plegridy is Beta interferon 1a (identical to Rebif and Avonex) with a Polyethylene Glycol attached to increase the apparent size of the molecule and decrease its clearance by the kidneys. This increases the availability of the interferon so you can take fewer injections. Pegylation (attaching a polyethylene glycol chain to a biological molecule) is a common trick used by pharmaceutical manufacturers to increase the duration of action of a biological agent for many disease states. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
Is it dangerous to drink alcohol when an MS patient has the JC virus? Answer: This wins the funniest question of the year. Drink away and enjoy :) Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
Is it common for a MS patient to experience weight loss while on Tecfidera ? Answer: Weight loss is not common on Tecfidera unless you have persistent gastrointestinal side effects like lack of appetite, nausea, abdominal pain, cramping and diarrhea. Since these side effects tend to either go away after several weeks or the person stops taking the drug, weight loss tends to be minimal. That being said, I did have a very stoic patient who continued on Tecfidera for many months despite persistent gastrointestinal side effects and that individual lost a lot of weight. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego #Tecfidera Here is My Question:
I am a 40 year old female. I had an episode of numbness and tingling and then a tremor about a year and half ago. We did MRIs of my spine and brain and they came back normal. All blood tests are normal. I saw an MS specialist and rheumatologist. All tests were normal. I just had an MRI brain a few months ago and it was normal. I still get tingling and numbness but it goes away quick. I have had bladder spams since this all started. Stiffness comes and goes in my legs. It is hard to climb stairs. I get tired easily. I was tested for Lyme disease and it was negative. Does MS take some time to show up? The MS specialist said the MRI is very definitive (99%) and she said MS is a very low possibility at this point. What can an expert tell me? Answer: It is quite uncommon for people with definite Multiple Sclerosis to have normal imaging of the brain and spinal cord over a several year interval. You should ask your doctor to tell you what he thinks is going on instead of telling you what you don’t have wrong with you. Prepare yourself with a list of questions and go to your meeting open minded and with someone you trust as a second ear. Try not to make up your mind about what is going on before you’ve heard completely from the doctor. If this is not satisfactory, it may be time to get a second opinion. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
Is it possible to have multiple sclerosis with out having your lower body affected? Answer: There is no rule that says the lower body must be involved for a person to have MS although it would be unusual for a person to experience MS for years without symptoms or examination findings eventually developing in the lower extremities. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego 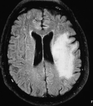 Here is My Question: If my MS is inactive how often do I need to have an MRI? I am claustrophobic and so MRIs are not fun and my doctor says I need one every 5 months? I haven't had any new symptoms so why do I need MRIs so often? Answer: This is a great question. How often a person needs to obtain a repeat MRI really depends on the circumstances. Let’s take the easy extremes to start:
This leaves everyone in between. Current recommendations are to repeat MRIs of the brain only every year unless there is a specific reason to do them sooner; the exceptions include monitoring people with more active disease, monitoring patients in the first year of treatment with a disease modifying therapy and monitoring for the development of PML in high risk patients on Tysabri. Most asymptomatic MS disease activity is reflected by an MRI of the brain so the spinal cord is less important in most circumstances for monitoring. Of course, it is only useful to repeat MRIs to monitor MS if it is done correctly. Sadly this is usually not the case in most clinical setting. For this reason, MRIs tend to be most useful in the first 5 years after a diagnosis, when it is relatively easier to determine if there is anything new. In the near future we will be rolling out a way for people to ensure that useful information is obtained on repeat MRIs. Stay tuned to this site to learn more. As for claustrophobia, I hear you loud and clear. For diagnostic purposes an open MRI will usually suffice but for repeat image analysis closed systems are preferable. Most people do very well with a good dose of lorazepam (1.5 to 2.0 mg) or alprazolam (same dose) about an hour before an MRI. You will need someone to drive you home Good luck Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego Here is My Question:
When I get stressed my MS definitely acts up. What happens in my brain when I get stressed. Why does it make my MS worse? Answer: It is certainly true that chronic stress activates multiple sclerosis and stress management reduces MRI measures of MS activity and improves symptoms. David Mohr at Northwestern published clinical trial results in 2012 demonstrating a very significant reduction in both enhancing lesions and new T2 lesions (white spots) on the MRIs of people with MS randomized to 16 weeks of stress management. The exact mechanism responsible for the worsening of MS and other physical and mental health conditions with chronic stress is linked to the effects of chronic stress on the hypothalamic-pituitary-adrenal axis which is generally linked to chronic low level elevations in cortisol. Notice how I have specifically referred to chronic stress throughout this answer. Acute stress has a number of beneficial effects just like acute short courses of corticosteroids can be beneficial in MS patients. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego |
PLEASE NOTE: This information/opinions on this site should be used as an information source only. This information does not create any patient-HCP relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition.
Archives
March 2024
Categories
All
|