|
Roche Pharmaceuticals, the owner of Genentech, announced positive phase III study results of their anti-CD20 monoclonal antibody called Ocrelizumab yesterday. Ocrelizumab is a humanized monoclonal antibody targeting CD20 on mature B cells, whereas Rituximab is a Chimeric antibody (part mouse and part human) with the same target. This clears the way for FDA approval of Ocrelizumab by late 2015 or early 2016. The two phase III studies involved 1656 relapsing MS patients (both relapsing remitting and secondary progressive) randomized to either an Ocrelizumab infusion every 6 months (600 mg) or Rebif 44 mcg three times a week. Ocrelizumab significantly reduced relapse rates, new lesion formation on MRI and disability progression during the two years of the study compared to Rebif. Amazingly, serous adverse events associated with Ocrelizumab were not more common than serious adverse events with Rebif, a drug considered very safe and a first line therapy for MS. The most common adverse events with Ocrelizumab were infusion related reactions, which can be controlled with premedication. A phase III study of Ocrelizumab in primary progressive MS is still underway.
Why is this important? 1. Many people with MS who have benefited from Rituximab in the past or could benefit from it now are no longer able to receive it because of insurance restrictions. These study results open the way for FDA approval of this class of medication 2. Only one other MS medication (Lemtrada) has shown significant benefits on relapse rates, disability progression and MRI activity over 2 years when compared to a highly active first line DMT (Rebif). Remember, it is relatively easy to be better than placebo treatment. Not only is Ocrelizumab better than Rebif, it is relatively safe and well tolerated over 2 years of treatment. A full understanding of the relative benefits and risks of Ocrelizumab awaits final release of the actual study data for us to review, but the statements in their press release are very exciting. 3. Any treatment that can be administered as infrequently as every 6 months will be welcome to most MS patients 4. Depending on our review of the study data, this drug may benefit certain secondary progressive MS patients All are cause for celebration. Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program University of California San Diego  By Revere (Rip) Kinkel MD Director of the UCSD Multiple Sclerosis Program Fatigue associated with MS is one of the most complex symptoms to evaluate and treat. There are many reasons for this complexity but the ubiquitous experience of fatigue tops the list. How many of us with or without MS have NEVER experienced fatigue? Probably no one on earth. It seems that every peak and valley we achieve in life is accompanied by fatigue; when we are down and ill we experience fatigue, and when we reach the pinnacle of success and happiness our exuberance overwhelms us and leaves us fatigued. I once read that fatigue is the most common complaint of people presenting to their primary care physician. If fatigue is so universal it stands to reason that we can not all be describing the same symptom, and yet we use the same word for all our complaints: fatigue. It is said that the experience of fatigue in people with MS is qualitatively similar to the usual experience of fatigue but differs quantitatively in terms of the persistence and severity of the fatigue. While this is true, it still does not help with the evaluation and management of fatigue when it persistently interferes with your life. So how do MS specialists help you evaluate and manage your fatigue under these circumstances? This topic is so complex that it is best for you to remember 5 important rules to help you over time: 1. Fatigue in people with MS is usually multifactorial. This means that fatigue is usually caused by a multitude of related or unrelated processes, not all of which are directly or even indirectly related to your MS. For instance, the fatigue may be 50 % caused by depression, 25 % caused by sleep disruption from chronic low back pain, 10 % caused by medication and 15 % caused by the direct effects of MS on the brain ( what we call primary MS related fatigue). It is the job of your MS specialist to help you figure out what factors are contributing to your fatigue and how to best treat it. In the example provided, treatment of the patient’s depression, elimination of the offending medication and improvement in sleep could go a long way towards improving the complaint of fatigue. On the other hand treatment with amantadine or modafinil for primary MS related fatigue would probably have little lasting benefit. 2. Fatigue means different things to different people. To some people fatigue means malaise or lassitude. To others it means the experience of being excessively sleepy during the day. Some are describing the experience of exertional weakness or mental fog or both. And some are describing a combination of fatigue experiences. It helps to be very specific when describing your complaint of fatigue. If fatigue means you are dragging your right leg after walking 100 feet and this requires you to rest before continuing, treatment may include a drug like ampyra to improve electrical conduction in your nervous system. If fatigue means you wake up feeling poorly rested and find yourself falling asleep easily during the day, then it is far more appropriate to assess your sleep quality to direct your treatment. 3. The causes of fatigue will change over time and must be re-evaluated frequently. This is probably obvious, but requires stating explicitly. I see many people with MS who benefited from amantadine or modafinil early in the course of their MS but eventually find that it no longer works or doesn’t work again when restarted. As you get older there are more and more opportunities for problems to develop that can contribute to fatigue. These may be unavoidable problems like other medical conditions (hypothyroidism as an example) or the addition of medications that cause fatigue. The list of medications causing or worsening fatigue is almost endless and one of the main reasons your MS specialist must continually reassess your need for certain medications. 4. There is never one treatment for fatigue. Treatment requires a multidimensional approach. If you expect to take a pill and eliminate your fatigue, you will be disappointed. Even in circumstances where the cause of fatigue is known and curable-- for instance, hypothyroidism--returning to normal after curing the hypothyroidism will require dietary modifications for the weight gain and an exercise program for the deconditioning. This is even more essential for chronic neurological problems like MS. Treatment should initially focus on the most treatable causes of your fatigue. This may include evaluation and management of treatable conditions (e.g. anemia), the elimination of unnecessary medications, improvement in sleep and treatment of depression. This should be accompanied by dietary modifications and a structured graduated exercise program with or without work and leisure activity adjustments during the day. People with MS should be regularly reassessed with the potential addition of medications to treat primary MS related fatigue, beginning with amantadine and considering modafinil or other stimulants if the amantadine is not effective. 5. Establish meaningful goals for treating your fatigue. It is rare that we totally eliminate fatigue in MS, so it is important to establish specific goals with your MS specialist and your family. This will help guide treatment recommendations. #msfatigue #fatigue #multiplesclerosisfatigue #waystofightfatigue  By Revere (Rip) Kinkel MD Director of the Multiple Sclerosis Program Professor of Clinical Neurosciences University of California San Diego We spend so much time discussing alterations in sight and tactile sensations (e.g. pins and needles, burning sensations, electrical sensations, itching) in MS that we often forget that the other senses may be affected as well. I thought I would briefly discuss these for you today. Acute hearing loss during the course of MS is relatively rare, although I suspect it occurs far more frequently than the reported 10 % incidence would suggest. Hearing loss at the onset of MS is even less frequent (1%) and often suggests another disorder masquerading as MS. Hearing loss may occur in isolation but is more readily associated with the multiple sclerosis when accompanied by other brainstem symptoms and signs such as vertigo, weakness or sensory disturbance on one side of the body, facial weakness or sensory disturbance sometimes opposite the affected side of the body, or incoordination of a limb. Unilateral hearing loss is more suggestive of an MS related cause, but MS may also rarely cause bilateral hearing loss. Many patients report symptoms such as tinnitus or fullness in the ear that may fall short of “hearing loss”, but still negatively affects auditory function and quality. Hearing loss is almost always caused by inflammatory demyelination in the part of the brain called the brainstem where the auditory nerve (also called the eighth cranial nerve) enters the central nervous system, or in the auditory pathways within the brainstem. It is said that high frequency hearing loss is more common with involvement of auditory nerve entry zone and tract, whereas low frequency hearing loss is more common with involvement of the auditory brainstem pathways. When hearing loss occurs acutely in MS, it often recovers along with other symptoms of a relapse after treatment with high dose steroids. However, like other symptoms there are some people who recover very little and are left nearly deaf. Tests can be done to determine if the hearing loss is caused by a problem in the cochlea (the inner ear and therefore not caused by MS) or the brainstem (more likely related to MS) but these tests are rarely necessary in a person known to have MS who experiences hearing loss. Altered smell and taste are reported more frequently in people MS (up to 2/3’s of people with MS may experience diminished smell perception and discrimination). Altered smell may even be a presenting symptom of MS, presenting either as diminished ability to smell (hypoguesia) or unpleasant abnormal smells (odors misinterpreted as smelling like gasoline, for instance). Rarely, patients will present with both altered smell and taste suggesting another problem such as a viral infection or a consequence of smoking. Altered taste can take many forms including inability to taste only sweet flavors, only sour or bitter flavors or both. The abnormal taste may affect only one or both sides and when it affects both sides the type of taste affected can differ on the two sides (i.e. sweet taste affected on one side and sour bitter tastes affected on the other side). In most situations people do not notice loss of taste when it affects only one side. Loss of or distorted smell is noticed with greater ease than loss of taste and often affects a person’s perception of smell as well. The proportion of people with MS who experience a decrease in smell perception and discrimination increases with the duration of disease and is related to amount of demyelination (white spots on MRI) in the inferior frontal lobes and temporal lobes of the brain. Not infrequently the diminished sense of smell is associated with problems controlling emotions or behavior, staying on task, planning activities or thoughts and seeing them through to the end. Both altered taste and smell have a large differential diagnosis. Common reversible causes of diminished smell include the common cold and other respiratory viruses, allergic rhinitis, chronic sinusitis, malnutrition and smoking. Other causes readily excluded by history, examination or imaging include head trauma, frontal lobe or suprasellar tumors, normal aging, Alzheimer’s disease and Parkinson’s disease. Diminished taste may also occur with common viral infections and with smoking but is particularly common with certain medications; for instance, most MS patients have noticed the bitter taste that occurs during the administration of high dose steroids to treat a relapse. Other correctable causes include vitamin B12 deficiency, zinc deficiency, and dry mouth either from medications or a disorder of salivary glands such as Sjogren’s syndrome. So the next time someone tries to tell you that MS does not affect hearing, smell or taste pull out this blog and educate them. But never assume a problem affecting these senses is related to your MS without a thorough evaluation by your MS Specialist. This week has been very busy, beginning with an NMSS society sponsored program in Boston to introduce MS Fellows (those being formally trained to become MS specialists) to the unique issues and concerns of people with advanced MS. Following my opening remarks and those of David Rintell, a wonderful psychologist in Boston at the Partner’s MS program, we were treated to a panel discussion with 4 caregivers of people with advanced MS. Three of the caregivers were spouses of a person with MS and the remaining person with MS was cared for by her mother and sister-in–law.
The challenges and stresses of their day-to-day existence was palpable in their demeanors and their frequent pauses to fight back tears and collect themselves before proceeding with their monologues. Each described the immense difficulty of accomplishing what to us is considered the most mundane of tasks; rolling their loved one over in bed, sitting them up, transferring them to a chair, standing them at the toilet, balancing them upright while pulling down their pants to sit on the toilet, cleaning and dressing them. Each described in vivid detail how dressing and toileting alone consumed a minimum of 2 hours every morning of their lives. Some of these caregivers did not qualify for personal care assistance because of their income level and never received any respite from their responsibilities; those that did qualify rarely experienced any significant respite or relief from their burden since they knew that no one could or would do as good a job as they are able to do. All of the caregivers acknowledged that their relationship with their loved one was no longer the same; as the disease advanced their loved one became dependent on them entirely and their prior partnership was no longer equal; changes in cognition and behavior often strained relationships further. Yet they persisted years on end caring for them, because they loved them. None could conceive of placing their loved one in a nursing home but all knew that a day could come when a nursing home was inevitable. I myself found it difficult to fight back tears while listening to their descriptions of daily life. At the end of the session, I asked each of them what would make their lives better. All of them felt that they needed more skilled caregiver assistance and support. So let me throw out an idea that may help us reach this goal; besides lobbying state governments for broader qualification criteria for personal care assistants (PCAs), I think caregivers should use a website like ours to develop requirements for PCAs, create a pool of PCAs in your region meeting these requirements (MS certified PCAs) that can be shared for MS care and use this site to communicate with each other to provide support and advice. We already have a caregiver blog but I think the MS HealthAllies site that will launch in the near future will also help with this endeavor. (if you haven't already signed up for the MS HealthAllies beta test please do so here...Click Here To Sign Up For MS HealthAllies Beta Test If you have any thoughts or ideas on this issue please share them with us. Lastly, the next time you meet someone who cares day in and day out for a loved one in the home, regardless of whether they have MS, give them a big hug. This little bit of support and affection does really help. -Rip Kinkel, MD I was reminded today at our weekly department grand rounds of an extremely important topic that MS specialists often forget; the benefits of folic acid supplementation in pregnancy age women. We spend so much time discussing the use of disease modifying therapies in pregnancy that we often forget about other equally common and well-known risks. It has been known for decades that folic acid supplementation in doses above 0.4 mg per day reduces the risk of neural tube defects such as spina bifida. What women often do not know is that by the time their pregnancy is confirmed, it is often too late to start this supplementation, since neural tube closure is an early event in embryogenesis (first 25 days). More importantly, at least 40 % of pregnancies are not planned in advance.
Why is this topic so important in woman of childbearing ages with MS? Well, one of the most common class of medications used to treat MS related symptoms are the anti-epileptic drugs (AEDs) such as gabapentin, valproic acid, carbamazepine, lamotrigine, phenytoin, primidone and topiramate. We use these drugs to treat MS related pain syndromes, migraine headaches, mood disorders and even the main disorder for which they were developed, seizures. This class of medication, particularly valproic acid, has been associated with a number of major congenital malformations (MCM) and, more recently, disorders affecting behavior and learning including autism spectrum disorders. The risk is even higher with use of more than one of these medications at a time. While most of the data supporting the association of certain AEDs with birth defects come from Epilepsy Pregnancy Registries, there is little reason to believe that this data would not apply to women using these medications for other indications. The reason for the increased risk of birth defects is clear with certain enzyme inducting AEDs such as phenytoin, carbamazepine and the barbiturates (primidone and phenobarbital), all of which cause a reduction in folic acid levels. For valproic acid it has been suggested that the drug interferes with folic acid metabolism. Other more recently introduced AEDs such as gabapentin, lamotrigine, oxcarbazepine and zonisamide have no significant effect on folic acid metabolism and the data on MCM is mixed. Yet most epilepsy specialists recommend folic acid supplementation in all women taking these drugs. So what should you do with this information if you are (a woman) women of childbearing potential regardless of whether you are on birth control? (Birth control can fail)
While the use of folic acid supplementation will not guarantee a child without birth defects, you can at least know you are doing something to reduce this risk. If you have daughters or grandchildren of childbearing ages, please pass this information along. -- Rip Kinkel, MD ECTRIMS Meeting Boston MA
September 10,2014 As I return to Boston for the start of the largest international MS meeting of the year, my thoughts have turned to the many wonderful resources that were and still are available to patients and their families in this area. From the many comprehensive MS Centers to the outstanding universities and research labs, Boston is truly an amazing place for people with MS. But one additional Boston area resource that is available in very few other locations around the country and often helpful to the many women with MS is a store in Brookline called Good Vibrations. As the name suggests, some may call this a sex shop but it is unique among enterprises of this nature with it’s attention to the needs of women (as well as LGST couples) and it’s focus on education. The staff are provided with extensive training and I’ve never heard of customers feeling uncomfortable with either the location or the store atmosphere. I’ve even heard of mothers and daughters visiting the shop together. Their emphasis on education is remarkable with a staff sexologist, Carol Queen PhD, available. In a world where the management of sexual dysfunction seems confined to improving erections in men, and medical doctors are still of little help to women with sexual dysfunction, it is good to know that there are resources available to women with these problem. There are Good Vibration stores also available in San Francisco, California although I have no personal knowledge of these stores. If you know of similar resources available in your community, please comment so we can post this information for other patients and families. So with the ECTRIMS meeting now underway, take some time out to visit Good Vibrations if you live in the area and you think this may help. After all, a healthy sex life has been shown to benefit fatigue, pain, sleep disruption, mood and well being. I will now return to the meeting and provide updates later this week or next week on new management strategies that may be of benefit to you now or in the near future. Good Vibrations 308 Harvard St Suite A Brookline, MA 02446 goodvibes.com -Rip Kinkel, MD  “The main facts in human life are five: birth, food, sleep, love and death.” ― E.M. Forster “I wonder why I don't go to bed and go to sleep. But then it would be tomorrow, so I decide that no matter how tired, no matter how incoherent I am, I can skip on hour more of sleep and live.” ― Sylvia Plath, The Unabridged Journals of Sylvia Plath Why do we so often forget how to sleep, as we grow older? Even without a chronic disease like Multiple Sclerosis our lifestyles and the changes to our body with aging conspire to interfere with restful sleep. Ask any woman going through menopause about their sleep and you will hear frustrating tales of awakenings for a variety of reasons many unexplained. Even well before the onslaught of middle age, our lifestyles become a hazard to sleep; we find ourselves with too little time between work and family responsibilities to take proper care of themselves. We stop exercising regularly, eat poorly, worry excessively and consume various drugs, some prescribed and others like alcohol and nicotine used to melt away our stresses and the burdens of feeling overwhelmed. Bad habits are formed early and persist. As the quote by Sylvia Plath (by the way she is not a good person from whom you should take advice regarding sleep) implies, from a young age we learn to burn the midnight candle too often and attempt to emulate those who never seem to require sleep. As people grow older they often develop strange beliefs or habits that actually worsen their sleep; some come to believe that they cannot fall asleep without the TV on or without a sleep aid and never attempt to adjust their sleep behavior. Often the problem is simply a result of a chronically disrupted circadian rhythm, yet the person insists it is simply impossible for them to fall asleep before 2 or 3 am. For people with MS, the problems with sleep are all too often blamed on the disease and simple measures are not attempted to control the insomnia before resorting to sleep aides or treatment of MS related symptoms perceived to be interfering with sleep. The cure for insomnia in MS patients and the excessive daytime sleepiness that it creates begins with the doctor taking a good history and patient being receptive to changing their current sleep behaviors. First, without excessive daytime sleepiness there is rarely a problem that requires treatment. Some people just require less sleep as they grow older; fewer still never require much sleep, yet never experience problems with feeling excessive sleepy during the day. With this caveat in mind it is often useful to separate sleep problems into three categories: those associated with sleep onset insomnia, those associated with nocturnal awakenings and those without perceived insomnia or awakenings but clearly creating excessive daytime sleepiness. Sleep onset insomnia (failure to get to sleep initially) is most often due to acute stressors, anxiety, depression (unipolar or bipolar), drugs (e.g. alcohol, stimulants including nicotine), eating large meals too late, pain, spasms when lying supine, restless legs syndrome or a disrupted circadian rhythm. These problems tend to be easy to identify and solve although they often require a willingness to change sleep behaviors (see list below). Medication to help with sleep onset insomnia is sometimes needed but only for short-term use. Long term use of medications to help with sleep should only be used after a complete evaluation. The same problems associated with sleep onset insomnia may also be responsible for awakenings during sleep, although the list becomes even longer with the inclusion of nocturnal awakenings to urinate because of bladder dysfunction, the co-existence of other medical conditions that interfere with sleep (Diabetes, lung disease, congestive heart failure etc.) and nocturnal hypoventilation in more severely disabled MS patients. The third category, excessive daytime sleepiness without perceived awakening, is often the result of a primary or secondary sleep disorder (obstructive sleep apnea, narcolepsy, nocturnal myoclonus, periodic limb movements of sleep) although your sleep partner is often able to provide the key history of snoring, suddenly disrupted breathing or leg movements that interfere with their sleep! Nocturnal hypoventilation can also present with feeling un-refreshed, confused and anxious on awakening because of not getting enough oxygen during sleep. As you have probably guessed by now, there is rarely one cause for your interrupted sleep and excessive daytime sleepiness. MS itself is often associated with daytime fatigue, a similar concept, but patients rarely describe this “fatigue” as the kind of daytime sleepiness one experiences after a bad night of sleep. Instead, MS fatigue is usually described as malaise, lassitude or an inability to move or think further without rest, more often without the craving to sleep during the day. The difficulty in diagnosis arises when a person experiences both daytime primary MS related fatigue and excessive sleepiness from disrupted sleep. So how should you manage your disrupted sleep? First, determine if your circadian rhythm is disrupted. This is usually obvious if you chronically find yourself unable to sleep until the middle of the night and then feel exhausted during the day because of the need to get up sooner than you would like. You will need to follow the advice listed below to improve your sleep hygiene but you may also need help in resetting your body’s clock; some people find success in resetting their clock by taking 3 mg of melatonin (an over the counter medication available at almost any pharmacy or supplement store) 2 hours before you would like to go to sleep. If this does not work after a week discuss the problem further with your physician. Rarely, a sleep specialist is needed to help people with chronic idiopathic (meaning unknown cause) insomnia. Next, you will need to adhere to the following steps to improve your sleep hygiene. This can be surprisingly difficult since many of us break these rules with regularity.
Lastly, if your problem with sleep or excessive daytime sleepiness is not easily managed with these adjustments or you are unable to follow through with these suggestions because of your MS or other medical problems, you will need to discuss these problems further with your primary care doctor or MS specialist. Common additional solutions may require treatment of depression, treatments of bladder problems to limit nocturnal awakening to urinate and treatment of pain and nocturnal spasms. A good sleep history should be obtained; it is often advisable to obtain a polysomnogram (also called a sleep study) and possibly an MSLT (multiple sleep latency test) if there is any suggestion of a sleep disorder or if attempts at treatment the insomnia fail to cure your excessive daytime sleepiness. “Suenos con los angeles” -Rip Kinkel, MD 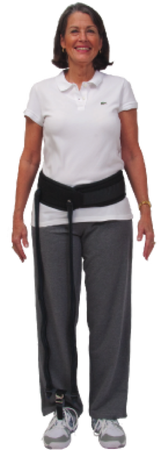 We have talked about devices that assist people with foot drop, but what do you do when your leg becomes so weak in the hip flexor or knee flexor muscles that you can not lift the leg well enough to bring it forward while walking or going up and down steps? Or if you fatigue so rapidly that you can not walk for more than a short distance? One possible solution is the Hip Flexion Assist Device (HFAD) shown in this picture. Essentially this is a strong weight lifting belt with two attached elastic bungee cords that attach to your shoe. Make sure you order the type with a horizontal connecting strap that goes behind the knee. The mechanical principle of the device is simple; extending the leg at the hip loads the bungee cord so that when you attempt to bring the leg forward, the cord contracts and helps lift the leg at the hip. Now it may not be the most attractive contraption but it does work and is relatively cost effective. You will need a prescription from your doctor and some training on the use of the device by your physical therapist. If you are interested in learning more, go to the following site for information: http://www.beckerortho.com/AffiliatedCompanies/BTMRehab/Btmhfad.html  So you’ve been told that you may have Multiple Sclerosis (MS). To borrow a common phrase, this is likely “freaking you out” and creating a great deal of anxiety. Take a breath, get comfortable and start reading. Rule 1: MS is rarely fatal and it is very rare for MS to cause disability in the first few years after diagnosis. You have time to get the medical opinions you need to make decisions and determine if anything else should be done to evaluate or treat your condition. This does not mean you should have to wait months to see a doctor specializing in this condition; months perhaps spent worrying unnecessarily. If you have an unnecessarily long wait to see a specialist ask your primary doctor for another referral. Rule 2: An important thing to know is that multiple sclerosis is often difficult to diagnose. Why? Well, there is no one test or exam that can definitively tell whether or not you have MS (nope, not even an MRI). Even after all tests and exams are done, some people cannot be diagnosed for years after the beginning of symptoms. The diagnosis of MS is based on symptoms and examination findings supplemented by diagnostic testing. The process of establishing a diagnosis is inherently complex requiring, at a minimum, the consultative services of a neurologist. A radiologist CAN NOT DIAGNOSE MS based on an MRI scan alone. A radiology report of an abnormal MRI scan indicating possible MS is often a cause of confusion, frustration and undue anxiety. The clinical criteria used to establish a diagnosis may sound complex but are really quite simple; a specialist needs to uncover specific symptoms or findings on examination that indicate inflammation in different parts of your central nervous system (i.e. the brain and spinal cord only) that occurred at different points in time. Very importantly, he or she must exclude alternative diseases capable of presenting in this fashion. Laboratory tests such as MRI scans, blood tests, spinal fluid analysis, and evoked potentials, supplement the clinical criteria and play a major role in confirming the diagnosis and eliminating alternative diagnostic possibilities. Of all these tests, the most important is an MRI scan but this alone can not be used to diagnose MS and must be interpreted by experts with caution. The common radiology report mentioning, “non-specific white matter changes” or “ white matter changes” consistent with MS means nothing by itself. The changes observed on the MRI scans of people with MS are very specific and can be classified for their specificity. For this you will require interpretation by an expert; unfortunately, most radiologists are not aware of this diagnostic criteria. Rule 3: Current diagnostic criteria for MS, revised in 2010, allow the diagnosis to be made at the onset of symptoms in certain people. Most people will need to be followed and obtain repeat MRI scans and clinical evaluations after the onset of their symptoms to determine if they have MS. In most cases the diagnosis can be established within 2 years. Those in whom it is more difficult to establish a diagnosis within 2 years tend to have a more benign prognosis. Rule 4: Certain syndromes (a syndrome is a collection of symptoms and findings developing in a typical pattern over time) are so commonly associated with MS that this diagnosis is strongly considered whenever the syndrome is observed in a person between the ages of 13 to 50. Often these syndromes have names attached to them, such as Optic Neuritis or Transverse Myelitis while others are referred to by less notable and less specific monikers such as Acute Brainstem Syndrome. Newly diagnosed MS cases over the age of 50, and very rarely under13, are certainly seen in our clinics but require a greater deal of care to exclude other conditions (e.g. strokes, degenerative diseases, leukodystrophies). Prior to the era of MR imaging, it was impossible to determine who would go on to develop typical MS and who would be found to have another diagnosis or never experience further neurological symptoms. Patients were considered, “At risk to develop MS” after experiencing typical symptoms for the first time, but were often not informed of this risk since the probability of MS was uncertain, and no therapies were available to reduce this risk or alter the future course of the disease. It took, on average, 5-years to establish a certain diagnosis of MS, a period of significant uncertainty and anxiety for many patients. MR imaging of the cranium and spinal cord, revolutionized this diagnostic process. First, MR imaging allowed clinicians to exclude many alternative conditions that mimic MS and respond best to appropriate therapies initiated as early as possible. Second, MR imaging now allows clinicians to establish a relative risk for the development of MS. For instance, over 50 % of patients have typical MS appearing MRI findings at the time of their first symptoms. The number and location of these abnormalities are strongly associated with the short-term risk of developing a clinical diagnosis of MS. Those individuals with highly typical findings are now considered at “high risk” to develop MS or given a diagnosis of MS immediately. Alternatively, those individuals without typical white matter abnormalities, especially those individuals with normal cerebrospinal fluid studies, are considered at low risk to develop MS with a 5 year diagnosis rate of less than 10 %. Therefore, imaging abnormalities at the onset of MS symptoms can be used to educate and counsel patients appropriately, and make decisions regarding early initiation of disease specific therapy. Rule 5: A definite diagnosis of MS does NOT mean a future marked by disability or loss of the ability to participate in the activities you love and find fulfilling. More than 25 % of people with MS never experience any significant disability without any treatment to alter the course of the disease. Those who require treatment experience significant reductions in symptomatic recurrences; it is increasing common for people to remain without significant disability for up to 3 decades or longer. Rule 6: Despite our current ability to establish a diagnosis of MS earlier and with greater certainty in many people, there are still cases where the diagnosis remains uncertain even with extensive testing. In these cases, the diagnosis should not be made prematurely; rather patients should be educated and counseled about diagnostic uncertainty from the onset. Education and follow-up plans, including repeat MR imaging studies every 6 to 12 months should be established. Repeat MR imaging will determine if characteristic white matter abnormalities have developed in the absence of new symptoms. Those people who experience continued difficulty coping with an uncertain diagnosis, even after appropriate education, may benefit from counseling to help ease the anxieties often associated with this process. Extra Credit: While establishing a diagnosis is beyond the scope of this discussion, it is useful to mention two common diagnostic errors. The first is diagnosing MS in patients with no definable neurological disease. The example provided in rule 1 is typical of this error. It is quite common for MS experts to see patients who have been diagnosed with MS by primary care physicians or other neurologists because of non-specific symptoms, such as general weakness, fatigue or tingling, at times supplemented by “minimal” changes on the MRI. By far the most common syndrome in this group of patients is recurrent parenthesis (i.e. usually described as pins and needles tingling sensations) in the extremities without any discernable abnormalities on neurological exam or diagnostic testing. The condition is so frequent that we often characterize the syndrome as "benign paresthesias". Often the sensory symptoms are accompanied by a history of chronic fatigue and/or chronic diffuse pain suggesting an overlap with fibromyalgia and chronic fatigue syndrome. Rarely, do these people develop MS; more importantly, a premature or inaccurate diagnosis of MS often interferes with the effective management of their condition. The second type of diagnostic error is incorrectly diagnosing MS in a patient who has some other neurological disease. The widespread use of MR imaging has helped to eliminate many of these diagnostic errors but they still occur, often as a result of misinterpretation of MR imaging findings or hasty diagnostic decisions made by a neurologist pressed for time. This type of error can be avoided by obtaining a second opinion with an MS Specialist and making sure you doctor reconsiders the diagnosis over time if unusual signs or symptoms should emerge. -Dr. Kinkel
 At the end of the day, people really want to know what is causing their symptoms and how to manage them. Whether you have definite MS or not, there will always be some degree of uncertainty; uncertainty regarding your risk of MS, uncertainty regarding the risk of future relapses, uncertainty regarding the risk of developing disability and uncertainty regarding your response to therapy, whether it be a drug, a dietary change or a lifestyle change. How you and your physician manage these uncertainties together over time defines the art of the doctor-patient relationship. If this process doesn’t work for you with your current doctor, discuss it openly with him or her and, if necessary, find a new doctor. Try to figure out what it is you require from a doctor to help you manage your chronic condition. As in the rest of life there will always be compromises you have to make but try to decide what you find to be most essential. Practical issues such as insurance coverage and distance from the doctor’s office are certainly important when it comes to narrowing down the list of doctors to consider, but should not be the basis of your decision. To me a doctor must first take the time to listen and understand your narrative (doctors call this the “chief complaint”), ask probing questions, explain their interpretation of the information gathered to gain further feedback and information and then put together a plan of action that you are capable of understanding and that clearly addresses your initial complaints. This is much harder than it sounds since often the person describing the “complaint”, is not only unaware of the cause but also unaware of the influence of seemingly random or apparently unimportant aspects of their life on this complaint. To give an example, I am often asked by patients to help them with their daytime fatigue, probably the most common symptom of MS. Many patients simply assume they only need a medication for this complaint and have learned that other patients take various medications for their fatigue. In fact, the causes of fatigue are extremely difficult to unravel and require a skilled history and dedicated follow-up evaluations after testing, activity adjustments and possible medication intervention to arrive at a satisfactory solution. As with most problems in medicine this is an iterative process: First, the complaint is identified and understood as best as possible generating a hypothesis that involves further testing or an intervention; second, the patient is educated about the intervention and given the means to carry out the intervention and track the progress; third, the patient is re-evaluated to determine the initial outcome to the intervention and generate further hypotheses leading to further testing or interventions; etc. This process requires skill, time, empathy and interactive resources. Anyone with a chronic condition wants to find not only a good doctor but a doctor with the support staff and associated medical professionals dedicated to working together on finding individualized solutions to problems. Here is a link to the NMSS to find a qualified specialist in your area: http://www.nationalmssociety.org/Treating-MS/Comprehensive-Care/Find-an-MS-Care-Provider/Partners-in-MS-Care In subsequent blogs we will be discussing these issues at length. I will always begin with the importance of education. Simply knowing the facts, or what is not known, is sometimes all that is needed. Where there are choices to be made I will try to outline them clearly, although it may become clear that I have a bias to express. Remember, an unbiased interpretation of data does not exist. What is important is whether the interpretation of the data is consistent with the known facts and your belief system. -Dr. Kinkel This blog was originally posted in August 2013. We are organizing the site and in order to move the blog we had to repost it. |
DISCLAIMER:
The medical information and opinions on this site are provided as an information resource only, and are not to be used or relied on for any diagnostic or treatment purposes. The information and opinions expressed do not create any patient-physician relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition. Archives
January 2020
Categories
All
|
- Home
- About Us
- Virtual MS Center
- News & Resources
- Seminar Registration
- Health & Wellness
- Blogs
- About MS
-
Symptoms
- Balance and Walking Issues
- Breathing/Respiratory
- Bowel Dysfunction
- Cognitive Dysfunction
- Crying/Laughing Uncontrollably (PBA)
- Depression and Anxiety
- Dizziness/Vertigo
- Dysphagia
- Fatigue
- Foot Drop
- Hearing or Smell or Taste Changes
- Heat Sensitivity
- Leg Weakness
- Loss of Hand Dexterity and Coordination
- Memory and Mutliple Sclerosis
- Migraines
- Numbness/Tingling/Altered Sensation
- Nystagmus and Oscillopsia
- Pain
- Sexual Dysfunction
- Sleep Issues
- Spasticity/Spasms/Cramps
- Speech/Swallowing
- Urination/Bowel Problems
- Vision
- MS Clinics
- MS Topics
- Register With Us
- Terms of Use/Privacy/HIPAA
- MS HealthCare Journey

 RSS Feed
RSS Feed
