|
I am often asked a variation on the same question, so I thought it best to write a blog that addresses the entire concept. The question is often phrased in one of the following ways:
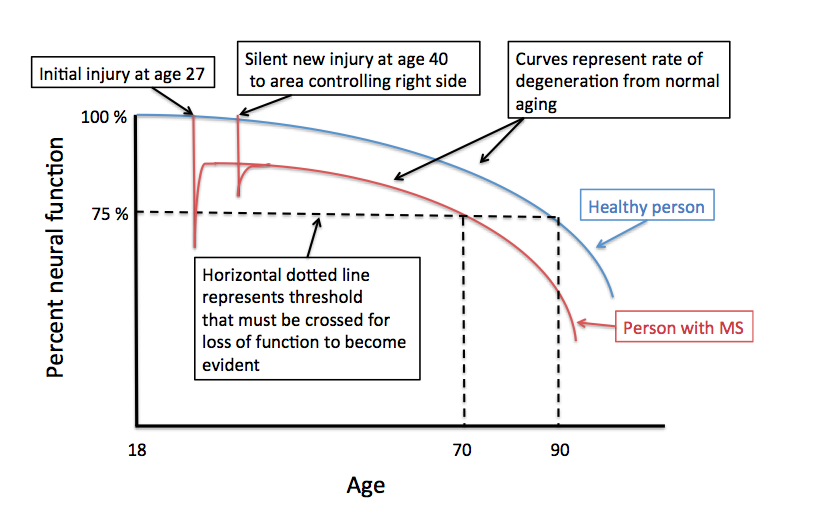
The theme of each question is identical; why after years of stability would someone with MS slowly get worse? There are, of course, several possibilities; it is most important for an individual with this concern to consult with an MS specialist or neurologist to determine the most likely reason for this delayed worsening after many decades of stability. One common cause is that the person has developed a new problem unrelated to MS, such as cervical spondylosis; this is a form of arthritis that can cause compression of the spinal cord with progressive walking difficulties often with stiffness and limited range of motion in the neck and neck pain that migrates into one or both arms. Many other reasons for delayed onset of neurological symptoms in an MS patient exist and require an evaluation to sort out. Another possibility is that the individual is developing secondary progressive MS; in some MS Clinics when this occurs after a single attack, the MS course is referred to as, “single attack onset progressive MS”. Determining if this is the cause of the worsening can be difficult and often requires years of observation for the clinician to be sure. More commonly, a person develops secondary progressive disease after experiencing more typical relapsing remitting MS earlier in life. The years of relatively stability without relapses before the onset of progressive worsening is not unusual, as relapses tend to get rare as you get older. The real question is what is happening during those years or even decades of stability? To answer this question in a manner that is easier to visualize I created the figure to go along with this blog. The Y-axis represents percent neural function and the X-axis is age. The figure begins at age 18 after the conclusion of normal development; at this time you should have 100% neural function assuming no injuries during development and adequate enrichment (diet, exercise, education, nurturing). The blue curve represents the gradual decline in neural function with age. This decline is probably not linear and is certainly affected by many life events as well as illnesses and chronic diseases.
Eventually, a normal healthy individual crosses a certain threshold of declining neural function, represented by the horizontal dashed line, and is no longer able to compensate well. In the example provided this occurs after the age of 90. I’ve labeled the threshold as 75% of normal neural function, but this is an arbitrary percentage; the threshold may be lower or higher or variable by region depending on a number of factors including physical and cognitive enrichment during development and ongoing physical, cognitive and social activity throughout adult life. We refer to these factors as passive and active neuronal reserve, respectively. Most studies indicate that active neuronal reserves, or your physical, cognitive and social activities in adulthood, are the most important in determining the affects of normal aging and the outcome from chronic neurologic disease like MS. The red curve represents a theoretical MS patient who experiences their first neurological symptoms at the age of 27; let’s say this causes left sided weakness. At the time of this attack (or exacerbation) the area of the nervous system responsible for the left sided weakness is temporarily injured and neural function declines below the 75 % threshold. This causes the patient to experience the behavioral manifestation of this decline in neural function (e.g. left sided weakness). In the example provided complete recovery of this behavioral manifestation of the neural injury (the left sided weakness) occurs even though the area is no longer able to provide the same level of neural function as a normal individual (i.e. the red line does not return to the blue line). This recovery occurs because of partial injury at onset, resolution of inflammation, remyelination and repair and neural plasticity (other areas of the brain taking over the behavioral function of the injured area or new connections forming from the injured area or both). In this same example the patient is remarkably stable and does not experience any further injury from MS until the age of 40. This time the injury does not cross the threshold and no symptoms occur, even though the area involved normally controls right-sided strength. An MRI may or may not show a new area of involvement and tissue recovery occurs once again. As we now trace out the red line while the person ages, we notice that the line crosses the 75 % threshold at an earlier age (age 70) than the healthy person represented by the blue line (age 90). At this age the MS patient can expect their left sided weakness to return and they will now slowly develop new right-sided weakness from the prior silent injury at the age of 40. How can this be prevented? One way is to prevent further injury from MS by using effective disease modifying therapies. The best way to shift the threshold line lower and therefore prevent the onset of declining neural function with age is to increase your active neuronal reserve. This is done by remaining healthy and actively involved with life through regular physical exercise, cognitive activity -particularly learning new skills- and remaining engaged socially. Now you know why I continually harp on the importance of remaining active in all these domains of life. Rip Kinkel, MD
0 Comments
Leave a Reply. |
DISCLAIMER:
The medical information and opinions on this site are provided as an information resource only, and are not to be used or relied on for any diagnostic or treatment purposes. The information and opinions expressed do not create any patient-physician relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition. Archives
January 2020
Categories
All
|
- Home
- About Us
- Virtual MS Center
- News & Resources
- Seminar Registration
- Health & Wellness
- Blogs
- About MS
-
Symptoms
- Balance and Walking Issues
- Breathing/Respiratory
- Bowel Dysfunction
- Cognitive Dysfunction
- Crying/Laughing Uncontrollably (PBA)
- Depression and Anxiety
- Dizziness/Vertigo
- Dysphagia
- Fatigue
- Foot Drop
- Hearing or Smell or Taste Changes
- Heat Sensitivity
- Leg Weakness
- Loss of Hand Dexterity and Coordination
- Memory and Mutliple Sclerosis
- Migraines
- Numbness/Tingling/Altered Sensation
- Nystagmus and Oscillopsia
- Pain
- Sexual Dysfunction
- Sleep Issues
- Spasticity/Spasms/Cramps
- Speech/Swallowing
- Urination/Bowel Problems
- Vision
- MS Clinics
- MS Topics
- Register With Us
- Terms of Use/Privacy/HIPAA
- MS HealthCare Journey

 RSS Feed
RSS Feed
